Maternal and paternal ages are highly correlated with relatively little variability in the age difference between the two parents. Women are pregnant at age 35 or older are often referred to as “advanced maternal age.” They may be told that they should have a labor induction or C-section at 39 weeks, solely because of their age. Woman’s age of 35 and older is considered as one of the key points in determining whether or not she will need advanced medical care during pregnancy due to a potential increase in pregnancy risk. Advanced paternal age is considering as a risk factor in pregnancy. Advance paternal age is defined as a father over 40 years of age. Studies showed that accumulation of chromosomal aberrations and mutations during the maturation of male germ cells are responsible for increasing risks of certain conditions with advancing paternal age. The amount of DNA damage in sperm of men aged 36–57 is three times that of men <35 years.
The key to a healthy pregnancy at any age starts with learning all you can about prenatal and pregnancy care – from preconception to postpartum.
A Woman’s Age and High Risk Pregnancy
There is no precise age when a woman becomes more susceptible to pregnancy complications. The age of 35 years is often used as a cutoff point, especially if it’s the first pregnancy. However, do not expect that at age of 45 years, your risk has suddenly changed. Rather, it’s a gradual process which accelerates around 35 years of age.
The good news is that most women who are older will get pregnant and deliver a healthy baby, though you should be aware of an increased risk of infertility and certain complications both to you and the baby once you do get pregnant.
Getting pregnant as you get older becomes more difficult. As a woman reaches her late 30s and early 40s, the risk of infertility and miscarriage significantly starts to rise. Studies have shown that infertility rates increase by about 3% for each year beyond 35.
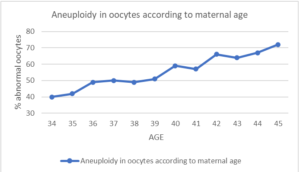
Women over 35 also have an increased risk of miscarriages mostly related to an increase in chromosomal anomalies among older women. Fetal chromosomal abnormalities may be caused by a nondisjunction phenomenon that occurs in the period of meiosis during maternal oogenesis, which has been reported to have a direct association with maternal age. Therefore, pregnancy in advanced age is a critical risk factor for fetal chromosomal abnormalities.
Currently, fetal chromosomal abnormalities due to maternal age have been reported to include trisomy 21, trisomy 18, trisomy 13, triple X syndrome, and Klinefelter’s syndrome.
As the percentages of pregnancies in women of advanced age have increased, there has been increasing demand for prenatal genetic counseling that helps to predict the risk of fetal chromosomal abnormalities depending on age.
About 10% of women over 35 have high blood pressure before pregnancy, and it complicates 10 to 20 percent of pregnancies in women over 35. Hypertension may also worsen during pregnancy, further increasing the risks for mother and baby. High blood pressure poses some risks to mother and baby and includes problems with the placenta and with the growth of the fetus.
There is also a higher incidence of gestational as well as overt diabetes in older women than in younger women, although the exact cause is unknown. Women with diabetes are at greater risk for pregnancy loss and a condition in which a fetus grows too large (macrosomia), and they are more likely to give birth by cesarean delivery.
In addition to high blood pressure and diabetes, complications of the kidneys, heart, liver and other organs also increase with age and could make pregnancy more at risk.
What are some health risks with advanced maternal age?
As women age, they are more likely to suffer from diseases and conditions associated with aging, such as miscarriage, diabetes, high blood pressure, and arthritis. Some of these conditions and the age of the mother, in general, may increase the risk of the following:
- Ectopic pregnancy
- Hypertension and Preeclampsia
- Congenital abnormality
- Heart Disease
- Chromosomal anomaly
- Kidney Problems
- Preterm labor and delivery
- Abruptio placentae
- Fetal growth restriction
- Placenta previa
- Stillbirth
- Cesarean section
- Cancer
- Maternal death
If you are older and become pregnant, you can expect that your doctor will probably monitor your pregnancy closer than that of a younger woman.
If you have a choice, see a doctor such as a maternal-fetal medicine (MFM) specialist who has experience with women of advanced age and high-risk pregnancies also you can see a certified genetic counselor in order to know the risk related to your age and the available genetic testing.
With advanced maternal age comes an increased chance of fraternal twin pregnancy. In addition to age, the number of pregnancies also comes into play. For example, if a woman over 35 becomes pregnant and has had four pregnancies prior to the current pregnancy, she is three times more likely to conceive fraternal twins.
Several studies have shown a relationship between preterm birth (PTB) and advanced maternal age. Their risk of preterm birth was 20 percent higher when compared to those aged 30-34 years.
The two most common invasive tests for women of advanced maternal age are CVS and amniocentesis. The risk of complications from these tests is less than one percent. The tests are often done as a follow up when a cell-free DNA blood test is abnormal.
Over the last decade, both amniocentesis and CVS have been mostly replaced as diagnostic screening tests by so-called “noninvasive tests” that can provide information on risks of the fetus having certain chromosomal conditions. If the cell-free DNA test is abnormal, then a diagnostic test such as amniocentesis or CVS is recommended.
- Cell-free DNA, a simple a blood test done as early as 10 weeks
- Nuchal translucency screening: a test done between 11 and 15 weeks that includes both a sonogram and a blood test. The blood test checks for levels of two substances: pregnancy-associated plasma protein-A (PAPP-A) and human chorionic gonadotropin. A special ultrasound, called a nuchal translucency screening, measures your baby’s fluid at the back of your baby’s neck, the neck’s thickness.
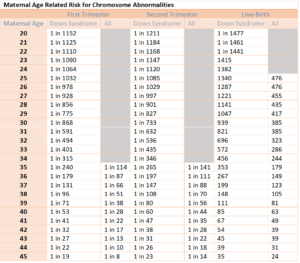
One of the most notable pregnancy risks for women of advanced maternal age is Down syndrome. Down syndrome is a chromosomal defect thought to be associated with aging eggs. By the age of 40, about one in 100 women are at risk of having an infant with down syndrome. Past the age of 40, the risk of down syndrome increases exponentially. By the advanced maternal age of 49, about one in 12 women are at risk. Doctors will often recommend the cell-free DNA test as an initial screening tests, and then recommend an amniocentesis or chorionic villus sampling (CVS) as a diagnostic test to determine the risk of Down syndrome in the fetus.
How does paternal age affect a baby’s health?
Studies suggest that a father’s age at the time of conception (paternal age) might pose health risks for a baby. However, this field of research is still relatively small, and results have been mixed. More research is needed.
Studies have shown that when paternal age is over 40, there might be a small increase in the risks of adverse pregnancy outcomes or risks to children’s health, including:
- Pregnancy loss. Advanced paternal age might be associated with a slightly higher risk of pregnancy loss before week 20 of pregnancy (miscarriage) or stillbirth.
- Rare birth defects. Older paternal age might slightly increase the risk of certain rare birth defects, including defects in the development of the skull, limbs, and heart.
- Research shows a link between older paternal age and an increased frequency of autism spectrum disorder.
- Studies suggest an older paternal age might increase the risk of the severe mental disorder schizophrenia and might be associated with earlier onset of schizophrenia symptoms.
- Childhood acute lymphoblastic leukemia. Older paternal age might be associated with a slightly increased risk of childhood acute lymphoblastic leukemia, a cancer that results in abnormal white blood cell production
- Spontaneous miscarriage rates are twice as common in partners of men age 50 years or older.
- Early births (< 32 weeks) and fetal deaths are twice as high in older compared to younger fathers.
Single gene disorders in offspring linked to paternal age
- Achondroplasia
- Apert syndrome
- Bilateral retinoblastoma
- Crouzon syndrome
- Fibrodysplasia ossificans
- Gardner Syndrome (Adenomatous Polyposis)
- Hemophilia A
- Lesch Nyhan syndrome
- Marfan syndrome
- Multiple Endocrine Neoplasia 2A,2B
- Neurofibromatosis 1
- Oculodentodigital syndrome
- Osteogenesis imperfect
- Pfeiffer syndrome
- Polycystic kidney disease
- Thanatophoric dysplasia
- Treacher-Collins syndrome
- Tuberous sclerosis
- Wardenburg syndrome
Birth defects in offspring associated with advanced paternal age
- Tracheoesophageal Fistula
- Atrial Septal Defect
- Ventricular Septal Defect
- Diaphragmatic Hernia
- Cleft Palate and Cleft Lip
- Pulmonary Stenosis
- Spina Bifida
Cognitive disorders in offspring associated with advanced paternal age
- Alzheimer’s Disease (AD)
- Attention Deficit Disorders (ADHD)
- Autism and Autism Spectrum Disorder
- Bipolar Disorder
- Dyslexia
- Schizophrenia
What Should You Do?
Men should understand that they too have a “biological clock” and proceed to become fathers with caution. Still, you should know that the overall risk is still quite low. And, currently, there is no testing to assess the risk beforehand. For concerned individuals, the pregnancy should be treated like a “high-risk” pregnancy, and the mother should have the appropriate prenatal screenings and tests that women receive for a high-risk pregnancy.
Now you call one of our genetic counselor and get a free counselling session.




